Cracks on Tongue and Vitamin Deficiency: Causes, Treatments, and Tips
A cracked tongue can be unsettling, especially when it seems to appear out of nowhere. Medically known as a fissured tongue or lingua plicata, this condition produces visible...
Written by Agnes Markovic
Read time: 9 min read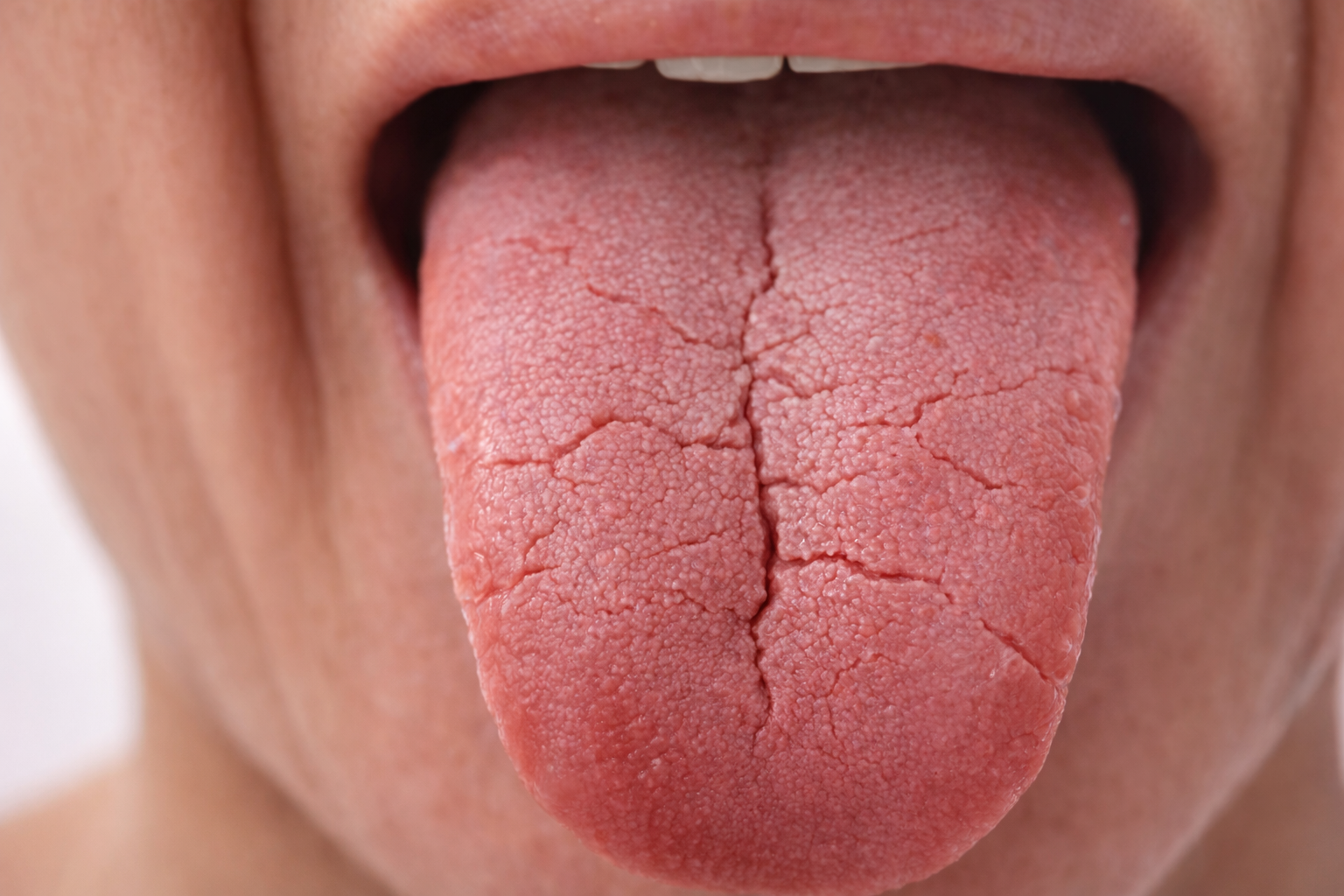
A cracked tongue can be unsettling, especially when it seems to appear out of nowhere. Medically known as a fissured tongue or lingua plicata, this condition produces visible grooves, splits, or furrows on the surface of the tongue that vary in depth and pattern. While some people are born with fissured tongues and never experience a single symptom, others develop cracks later in life that come with pain, burning, or swelling.
One of the most frequently overlooked causes of tongue fissures is nutritional deficiency. Vitamins and minerals play a direct role in maintaining the health of the oral mucosa, and when the body runs short on specific nutrients, the tongue is often one of the first places to show it. Research published in the National Institutes of Health (NIH) has documented a connection between fissured tongue syndrome and lower levels of vitamin B12, folate, and ferritin.
This article breaks down which vitamin deficiencies cause cracks on the tongue, how to identify deficiency-related fissures, the best treatment approaches, and practical at-home remedies that support tongue health. All recommendations are grounded in clinical evidence and dental best practices. Whether you have noticed new grooves forming on your tongue or have been living with fissures for years and are now experiencing new symptoms, the information here will help you understand what may be happening and what steps to take next.
What Is a Cracked or Fissured Tongue?
A fissured tongue is characterized by one or more grooves running along the surface of the tongue. These grooves can be shallow or deep, and they may radiate outward from a central fissure or appear in an irregular, branching pattern. The condition affects an estimated 5% to 7% of the general population, and its prevalence increases with age.
Fissured tongues can be broadly categorized as congenital or acquired. Congenital fissures are present from birth or early childhood and are considered a normal anatomical variation. They tend to be painless and remain stable over time. Acquired fissures, on the other hand, develop later in life and can indicate an underlying condition, nutritional deficiency, or chronic irritation.
The location of the cracks can sometimes offer clues about the cause. A central groove running down the midline is often congenital or linked to dehydration, while cracks along the edges of the tongue may result from chronic mechanical irritation such as teeth clenching. Fissures accompanied by redness, swelling, or a burning sensation are more likely to have a systemic cause, including nutrient shortage.
Several medical conditions are associated with a fissured tongue, including geographic tongue, Melkersson-Rosenthal syndrome, Down syndrome, and psoriasis. However, in many cases, the underlying factor is far simpler: the body is missing key vitamins or minerals that the oral mucosa depends on to stay healthy.
What Vitamin Deficiencies Cause Cracks on the Tongue?
Nutritional deficiencies are among the most treatable causes of tongue fissures. When the body lacks certain vitamins and minerals, the delicate mucous membranes of the mouth become vulnerable to inflammation, thinning, and cracking. The deficiencies most commonly associated with tongue fissures are outlined below.
Vitamin B12 (Cobalamin)
Vitamin B12 is essential for red blood cell formation, nerve function, and the maintenance of healthy mucous membranes. A deficiency can lead to glossitis, a condition in which the tongue becomes swollen, smooth, and inflamed. In some cases, glossitis progresses to visible cracks and fissures, often accompanied by a burning or sore sensation.
A study cited by Medical News Today found a direct link between a cracked tongue and vitamin B12 deficiency. Pernicious anemia, an autoimmune condition that impairs B12 absorption, is one of the most common systemic causes of B12-related oral changes.
Food sources rich in B12 include beef, liver, sardines, salmon, eggs, dairy products, and fortified cereals. Adults need approximately 2.4 micrograms per day. Vegans and vegetarians are at higher risk of deficiency because B12 occurs naturally only in animal products.
Vitamin B2 (Riboflavin)
Riboflavin plays a central role in energy metabolism and the health of mucous membranes throughout the body. Hallmark signs of riboflavin deficiency include painful cracks at the corners of the mouth (angular cheilitis), a magenta-colored tongue, and scaly patches on the scalp. Tongue fissures are a recognized oral manifestation of this deficiency.
Good dietary sources of riboflavin include milk, yogurt, cheese, eggs, lean meats, almonds, and enriched grains. The recommended daily intake is 1.3 mg for adult men and 1.1 mg for adult women.
Vitamin B3 (Niacin)
Severe niacin deficiency causes pellagra, a condition defined by the "four Ds": dermatitis, diarrhea, dementia, and, if untreated, death. A milder deficiency can produce oral symptoms well before full pellagra develops, including a swollen, red, or cracked tongue. Niacin supports tissue repair and cell turnover in the oral mucosa, and insufficient levels leave the tongue more susceptible to damage.
Niacin-rich foods include chicken, turkey, tuna, salmon, peanuts, lentils, and fortified breads. The recommended daily allowance is 16 mg for men and 14 mg for women.
Vitamin B9 (Folate)
Folate is critical for DNA synthesis and cell division, both of which are essential for maintaining the rapidly turning-over cells of the oral mucosa. Low folate levels impair mucosal regeneration, leading to a smooth, sore, and sometimes cracked tongue. A case study in the NIH's PubMed Central documented glossitis and fissured tongue in patients with folic acid deficiency linked to malabsorption syndromes.
Folate is found in dark leafy greens (spinach, kale, romaine), asparagus, Brussels sprouts, legumes, citrus fruits, and fortified grains. Adults need 400 mcg daily, with higher amounts recommended during pregnancy.
Iron
Iron-deficiency anemia is one of the most widespread nutritional deficiencies globally, and it has well-documented effects on oral health. A shortage of iron leads to thinning of the oral mucosa, making the tongue more vulnerable to cracks, soreness, and a pale or abnormally smooth appearance. The tongue may also develop a burning sensation, particularly at the tip and edges.
Iron-rich foods include red meat, organ meats, shellfish, spinach, lentils, chickpeas, tofu, and iron-fortified cereals. The recommended daily intake ranges from 8 mg for adult men to 18 mg for premenopausal women. Pairing iron-rich foods with vitamin C improves absorption.
Zinc
Zinc is essential for wound healing, immune function, and tissue regeneration. A zinc deficiency can slow the repair of damaged oral tissues, allowing minor irritation to progress into deeper grooves and fissures. Burning sensations and taste disturbances are also common in zinc-deficient patients.
Oysters are the most concentrated dietary source of zinc, followed by beef, crab, pumpkin seeds, cashews, chickpeas, and yogurt. The recommended daily intake is 11 mg for men and 8 mg for women.
It is important to note that tongue fissures alone do not confirm a nutritional deficiency. Painless, stable fissures that have been present for years are often genetic and entirely harmless. The presence of additional symptoms, such as burning, swelling, color changes, or soreness, increases the likelihood that a deficiency is involved. A blood test is the only reliable way to confirm a specific deficiency.
How to Tell if Your Cracked Tongue Is Caused by a Vitamin Deficiency
Not every cracked tongue points to a nutritional problem. The key is distinguishing between a benign, lifelong fissured tongue and one that has developed or worsened recently alongside other symptoms. There are several signs that suggest a deficiency may be at play.
A tongue that has become newly cracked or that is progressively worsening deserves attention, especially when accompanied by a burning or stinging sensation that intensifies with acidic or spicy foods. Changes in tongue color, such as an unusually pale, bright red, or magenta appearance, can also signal a nutritional issue. Swelling, smoothness (loss of the small papillae that normally cover the tongue), and persistent soreness are additional red flags.
Other clues may come from outside the mouth. Fatigue, weakness, brittle nails, hair loss, pale skin, and frequent mouth ulcers are all systemic symptoms that can accompany the same deficiencies responsible for tongue changes. If any of these signs are present alongside tongue fissures, a visit to a dentist or physician is warranted.
A dentist can examine the tongue, assess oral health, and refer for blood work to check levels of B12, folate, iron, zinc, and other relevant markers. Once the specific deficiency is identified, treatment can begin. For patients who want to stay on top of their oral health more broadly, routine dental visits are an opportunity to catch these changes early.
How to Treat Tongue Cracks Caused by Vitamin Deficiency
Treating a cracked tongue that stems from a nutritional deficiency involves two parallel strategies: correcting the underlying deficiency and managing the tongue symptoms directly. The most effective outcomes come from addressing both at the same time.
Step #1: Get a Professional Diagnosis
Self-diagnosing a vitamin deficiency based on tongue appearance alone is unreliable. A blood test ordered through a dentist, physician, or primary care provider can confirm whether levels of B12, folate, iron, zinc, or other nutrients fall below the normal range. Treatment plans should be based on confirmed results rather than guesswork.
Step #2: Adjust Your Diet
Dietary changes are the foundation of any deficiency correction plan. Prioritizing nutrient-dense whole foods is the most sustainable long-term approach. A useful daily framework includes:
Lean protein (poultry, fish, eggs, legumes) for B vitamins, iron, and zinc
Dark leafy greens (spinach, kale, Swiss chard) for folate and iron
Dairy or fortified plant milks for B12 and riboflavin
Nuts and seeds (pumpkin seeds, almonds, cashews) for zinc and B vitamins
Citrus fruits and bell peppers for vitamin C, which aids in iron absorption
Step #3: Consider Supplementation
When dietary intake alone cannot correct a deficiency, or when absorption is impaired (as in pernicious anemia or celiac disease), supplementation becomes necessary. The specific supplement, dosage, and form should be guided by a healthcare provider based on blood test results. Over-supplementation, particularly with iron, carries its own risks and should be avoided without professional oversight.
Step #4: Support Oral Hygiene
While the deficiency is being corrected, maintaining excellent oral hygiene helps prevent secondary complications. Food debris, bacteria, and fungi can accumulate in tongue fissures, increasing the risk of infection, bad breath, and further irritation.
Brush the tongue gently with a soft-bristle toothbrush twice daily
Use a tongue scraper to remove debris from deeper grooves
Rinse with an alcohol-free mouthwash to avoid irritating the cracked tissue
Stay well hydrated, as dry mouth worsens tongue cracking
Clinical literature, including a case reported in PubMed Central, has documented visible improvement in tongue fissures within approximately six weeks of dietary supplementation and B-complex injections. Recovery timelines vary depending on the severity of the deficiency and individual health factors.
Best Vitamin Supplements for Healing Cracks on the Tongue
Choosing the right supplement matters. Not all products are equally effective, and understanding which forms of vitamins and minerals the body absorbs most readily can make a meaningful difference in outcomes.
B-Complex Supplements
A B-complex supplement covers all eight B vitamins, including B2, B3, B6, B9, and B12, in a single daily dose. For patients with multiple borderline deficiencies, this is often the most practical option. Look for a product that contains methylcobalamin (the active form of B12) rather than cyanocobalamin, as methylcobalamin is more bioavailable and does not require conversion in the body.
Similarly, methylfolate (5-MTHF) is the preferred form of folate in supplements, especially for individuals who carry the MTHFR gene variant, which impairs the body’s ability to convert synthetic folic acid into its usable form. A quality B-complex should list the active forms of each vitamin on the label. Avoid products that rely heavily on fillers, artificial colors, or proprietary blends that obscure individual dosages.
Iron Supplements
Iron should only be supplemented after a confirmed deficiency, as excess iron can cause gastrointestinal distress, constipation, and, in serious cases, organ damage. Ferrous bisglycinate is generally better tolerated than ferrous sulfate and produces fewer side effects. Taking iron with vitamin C, such as a glass of orange juice, enhances absorption.
Zinc Supplements
Chelated zinc (zinc picolinate or zinc bisglycinate) tends to be better absorbed than zinc oxide. The standard supplemental dose for adults is 15 to 30 mg per day. Zinc competes with copper for absorption, so long-term supplementation may require monitoring copper levels.
Are There Specific Multivitamins That Help With Tongue Fissures?
A well-formulated multivitamin that includes adequate doses of the B-vitamin group, iron, zinc, and folate can serve as a reasonable baseline, particularly for people who suspect mild deficiencies across multiple nutrients. However, targeted supplementation based on blood work is almost always more effective than a broad-spectrum multivitamin. If a specific deficiency is identified, the relevant nutrient should be taken at therapeutic doses, which most standard multivitamins do not provide.
Where Can You Buy Vitamins for Tongue Health?
Vitamin supplements for tongue health are widely available at pharmacies, health food stores, and major online retailers. In the United States, chains such as CVS, Walgreens, Whole Foods, and Vitamin Shoppe stock a range of B-complex, iron, and zinc products. Online options include Amazon, iHerb, and manufacturer-direct websites. Look for third-party testing certifications such as USP, NSF, or ConsumerLab to verify product quality and label accuracy.
For patients with dental insurance, some plans cover nutritional counseling as part of preventive care. Check with your provider to see whether a consultation with a registered dietitian is included in your benefits.
At-Home Remedies for Cracked Tongue Due to Vitamin Issues
While correcting the underlying deficiency is the primary treatment, several at-home remedies can help manage discomfort, reduce the risk of secondary infection, and support healing. These measures are best used alongside professional care, not as a substitute for it.
Saltwater Rinses
A warm saltwater rinse (half a teaspoon of salt dissolved in eight ounces of warm water) is one of the simplest and most effective oral hygiene practices. Rinsing two to three times daily helps cleanse fissures, reduce bacterial load, and soothe irritated tissue. Saltwater rinses are gentle enough for daily use and do not carry the drying effects of alcohol-based mouthwashes.
Gentle Tongue Cleaning
Brushing the tongue with a soft-bristle toothbrush or using a dedicated tongue scraper removes food particles and bacteria that accumulate in the grooves of a fissured tongue. This is especially important for people with deeper cracks, where debris can become trapped and promote fungal growth, including oral candidiasis (thrush).
Hydration
Dehydration and dry mouth are contributing factors to tongue cracking. Drinking adequate water throughout the day, aiming for at least eight glasses, helps maintain saliva production and keeps the oral mucosa moist. Patients who take medications that cause dry mouth (such as antihistamines, antidepressants, or blood pressure drugs) should discuss saliva substitutes or stimulants with their dentist or physician.
Dietary Adjustments
Certain foods can aggravate a cracked tongue, particularly during the healing phase. Reducing or temporarily eliminating the following can help minimize discomfort:
Spicy foods (chili, hot sauce, pepper-heavy dishes)
Highly acidic foods and beverages (citrus juice, tomato sauce, vinegar-based dressings)
Very hot foods and drinks that can irritate exposed tissue
Alcohol, which dries out the oral mucosa and slows healing
At the same time, increasing intake of nutrient-dense foods that support the specific deficiency, such as leafy greens for folate and lean meats for B12 and iron, directly contributes to recovery.
Avoiding Tobacco
Smoking and chewing tobacco both damage the oral mucosa, impair blood flow to the tongue, and slow tissue healing. For anyone dealing with a cracked tongue, quitting tobacco is one of the most impactful steps they can take. Dentists can provide resources and referrals to cessation programs.
Probiotics and Oral Microbiome Support
Emerging research suggests that maintaining a healthy oral microbiome may support mucosal healing. Probiotic strains such as Lactobacillus reuteri and Lactobacillus rhamnosus have been studied for their potential to reduce oral inflammation and inhibit the growth of harmful bacteria and fungi in the mouth. While the evidence is still preliminary, incorporating probiotic-rich foods such as yogurt, kefir, sauerkraut, and kimchi may offer modest benefits alongside other treatments.
Probiotic lozenges designed specifically for oral health are also available at most pharmacies. These products are formulated to dissolve slowly in the mouth, delivering beneficial bacteria directly to the oral mucosa. They should be considered a complementary measure rather than a standalone treatment.
Keeping a Symptom Diary
Tracking what you eat and drink alongside your tongue symptoms can help identify triggers that worsen cracking or burning. Over time, patterns often emerge that allow you to adjust your diet and avoid irritants. Note the severity of pain or burning on a simple 1–10 scale each day, along with what you consumed, how much water you drank, and any supplements taken. This diary is also valuable information to share with a dentist or physician at your next appointment, providing them with concrete data to guide treatment decisions.
When to See a Dentist or Doctor About a Cracked Tongue
Most mild, painless tongue fissures do not require urgent medical attention. However, there are several situations where professional evaluation is important.
Schedule an appointment if you experience any of the following:
Tongue fissures that are new, worsening, or deeper than before
Persistent pain, burning, or stinging that affects eating or speaking
Changes in tongue color, such as an unusually red, pale, or magenta appearance
White or yellow patches on the tongue that could indicate a fungal infection
Sores on the tongue that do not heal within two weeks
Swelling or difficulty moving the tongue
Accompanying systemic symptoms such as fatigue, weakness, or frequent mouth ulcers
A dentist can perform a thorough oral examination, check for signs of infection or other conditions, and refer for blood work if a deficiency is suspected. Catching and treating nutritional deficiencies early prevents more serious complications down the line, including nerve damage from prolonged B12 deficiency.
The diagnostic process is usually straightforward. A complete blood count (CBC) can reveal anemia, while specific tests for serum B12, folate, ferritin (stored iron), and zinc provide a clear picture of nutritional status. In some cases, additional testing may be needed to determine why a deficiency exists, such as screening for celiac disease, pernicious anemia, or other absorption disorders that prevent the body from utilizing nutrients properly.
Patients who have undergone bariatric surgery, follow strict vegan or vegetarian diets, take proton pump inhibitors (PPIs) for acid reflux, or have a history of gastrointestinal conditions are at elevated risk for nutritional deficiencies and should mention these factors to their healthcare provider. Early testing in these groups can prevent tongue symptoms from developing in the first place.
Regular dental check-ups are one of the most effective ways to monitor tongue health over time. Dentists are trained to recognize oral signs of systemic disease, and a routine visit can catch changes that patients might not notice on their own. During a standard examination, the dentist will assess the tongue’s color, texture, and moisture level, check for swelling or lesions, and look for signs of infection in any existing fissures. This takes only a few minutes but can provide early warning of issues that deserve further investigation. Readers looking for guidance on finding the right provider or understanding what dental visits involve can explore resources on the Dental Reviewed blog.
Tongue Cracks and Nutrient Shortage Solutions: A Quick-Reference Summary
The table below provides a concise overview of the key deficiencies linked to tongue fissures, their primary food sources, and supplementation considerations.
Vitamin B12: Food sources include beef, liver, eggs, dairy, and fortified cereals. Supplement form: methylcobalamin. RDA: 2.4 mcg.
Vitamin B2: Food sources include milk, yogurt, eggs, almonds, and enriched grains. Supplement form: riboflavin or riboflavin-5-phosphate. RDA: 1.1–1.3 mg.
Vitamin B3: Food sources include chicken, tuna, peanuts, lentils, and fortified breads. Supplement form: niacinamide (lower flush risk). RDA: 14–16 mg.
Vitamin B9: Food sources include spinach, kale, legumes, citrus, and fortified grains. Supplement form: methylfolate. RDA: 400 mcg.
Iron: Food sources include red meat, shellfish, spinach, lentils, and fortified cereals. Supplement form: ferrous bisglycinate. RDA: 8–18 mg.
Zinc: Food sources include oysters, beef, pumpkin seeds, cashews, and yogurt. Supplement form: zinc picolinate. RDA: 8–11 mg.
Bottom Line
Cracks on the tongue are common, and in many cases, they are harmless. However, when fissures develop alongside pain, burning, swelling, or color changes, a nutritional deficiency is one of the most likely and most treatable causes. Deficiencies in vitamin B12, riboflavin, niacin, folate, iron, and zinc have all been linked to tongue changes in published clinical research.
The best approach starts with a professional diagnosis. A blood test can confirm which specific nutrients are low, allowing for targeted dietary changes and supplementation rather than guesswork. Supporting the healing process with good oral hygiene, hydration, and avoidance of irritants helps manage symptoms while the underlying deficiency is corrected.
If you have noticed new or worsening cracks on your tongue, do not ignore them. Schedule a visit with your dentist or physician, ask for blood work, and take the first step toward identifying and addressing the cause. Most patients see meaningful improvement within four to eight weeks of starting the right treatment.
This article is for informational purposes only and does not constitute medical advice. Always consult with qualified healthcare professionals for diagnosis and treatment recommendations specific to your situation.
Frequently Asked Questions
Can a cracked tongue heal on its own?
Mild fissures caused by temporary dehydration or minor irritation may resolve without treatment. However, cracks caused by a vitamin deficiency will typically persist or worsen until the underlying nutritional issue is addressed through dietary changes, supplementation, or both.
Is a fissured tongue always a sign of vitamin deficiency?
No. Many people have fissured tongues from birth as a normal anatomical variation. Genetic fissures are painless, stable, and do not require treatment. Deficiency-related fissures tend to appear later in life and are accompanied by symptoms such as pain, burning, or changes in tongue color.
How long does it take for tongue fissures to improve after treating a deficiency?
Most patients notice improvement within four to eight weeks of consistent treatment, including dietary adjustments and supplementation. Severe or long-standing deficiencies may take longer. A case reported in PubMed Central showed marked tongue improvement after approximately six weeks of B-complex supplementation combined with dietary changes.
Can children get cracked tongues from vitamin deficiency?
Yes, although a fissured tongue in children is more commonly genetic. Nutritional deficiencies can occur in children with restrictive diets, absorption disorders, or chronic illness. A pediatric dentist or pediatrician can evaluate tongue changes in children and order appropriate testing if a deficiency is suspected. For parents seeking age-appropriate oral health guidance, the Dental Reviewed blog covers pediatric topics in detail.
Should I take supplements without a blood test?
Taking a general multivitamin at standard doses is generally considered low-risk for most adults. However, self-prescribing high-dose individual supplements, particularly iron, without confirming a deficiency through blood work, is not recommended. Excess iron intake can cause gastrointestinal problems and, over time, organ damage. A blood test provides the clarity needed to supplement safely and effectively.
Can stress cause a cracked tongue?
Stress does not directly cause tongue fissures, but it can contribute indirectly. Stress-related behaviors such as teeth grinding (bruxism), tongue thrusting, and jaw clenching can irritate the tongue and worsen existing cracks. Stress can also disrupt eating patterns and nutrient absorption, potentially contributing to deficiencies that affect oral health.
What is the difference between a fissured tongue and geographic tongue?
A fissured tongue has grooves or cracks on its surface, while geographic tongue (benign migratory glossitis) produces smooth, red patches surrounded by slightly raised white borders that shift in location over time. The two conditions can coexist, and both are generally benign. However, geographic tongue is more commonly associated with discomfort when consuming acidic or spicy foods. For guidance on managing tongue-related oral conditions, dental professionals can provide condition-specific recommendations.
Are cracked tongues contagious?
No. Fissured tongue is not an infectious condition and cannot be transmitted from person to person. It results from genetic factors, nutritional deficiencies, aging, or associated medical conditions, none of which are contagious.